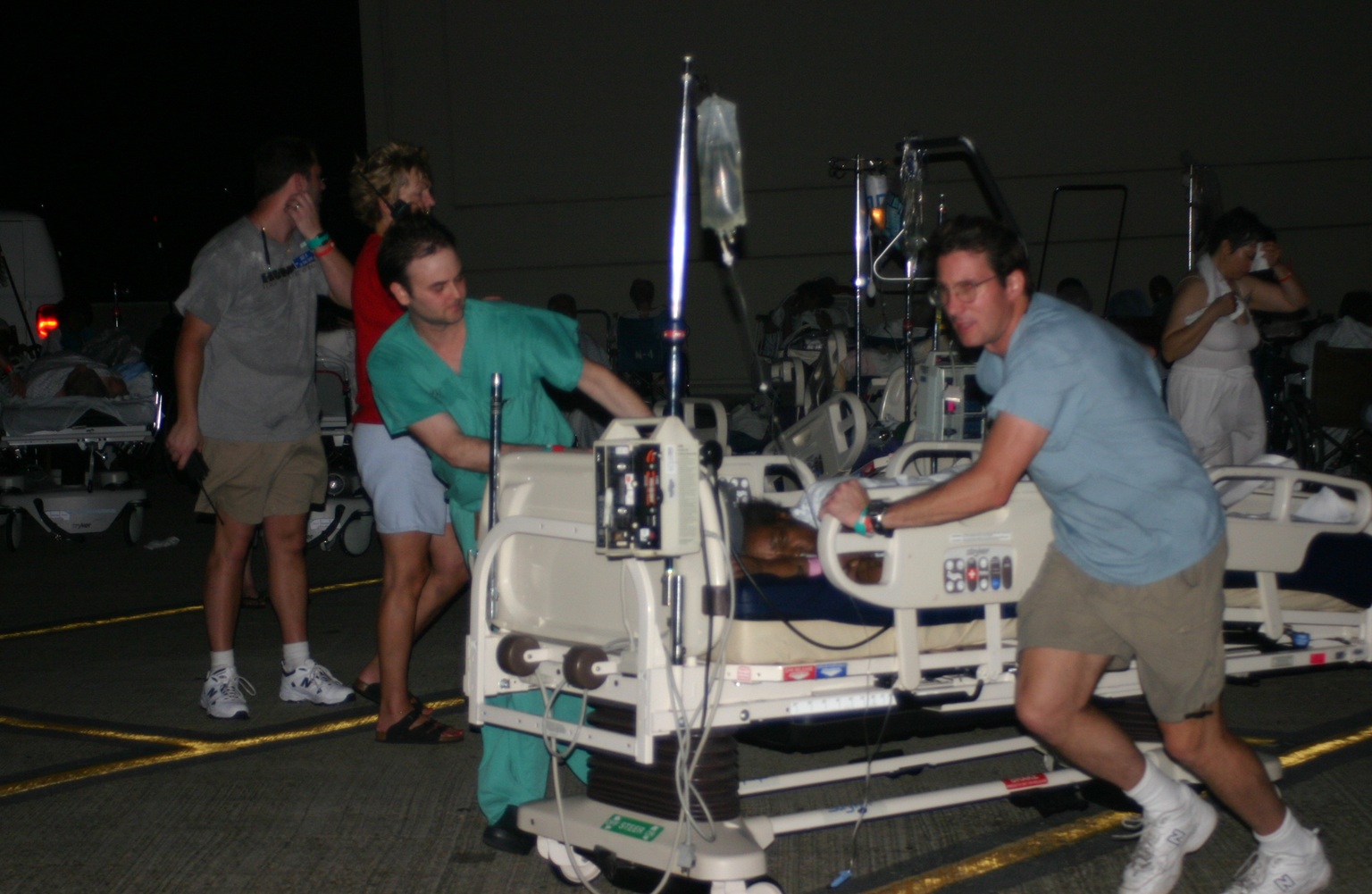
Hours after Hurricane Katrina made landfall in New Orleans. Hours after Touro Infirmary lost power. Hours after gas trucks delivered enough product to support the backup generators at the hospital, only to see those generators fail. And hours after it became clear the hospital would have to evacuate its 238 patients — along with the approximately 1,700 staff members and their families who had come there seeking shelter — the new CEO, who had only been on the job a week, made a quick decision.
Les Hirsch decided he was going to lead.
“I had my own moment of truth,” he told BINJE. “I processed it, and I thought to myself: There’s no standing on the sideline. I decided that if I didn’t take leadership then, then I could never lead. So, I did.”
Hirsch, a Jersey native who is now the CEO of Saint Peter’s Healthcare System in New Brunswick, said board members and other hospital executives at Touro told him later that they were grateful — but also surprised — that he even chose to stay.
After all, the unfathomable destruction that occurred when the levees broke — followed by civil unrest that those who weren’t there are better off not knowing about — were enough to test the strength of generational residents, let alone a newbie to the area.
Hirsch said he never wavered.
After seeing what he called an unprecedented failure of government at the local, state and federal levels, a nearly biblical loss of life and property damage from the flood, and a massive drop of protective and social services, Hirsch said there was no other option.
It was an incredible challenge.
Touro had no power, which meant patients on ventilators needed to be bagged by hand. It had no running water, which meant toilets could not be flushed. And the lack of electricity meant no air conditioning in the stifling heat and humidity of the city, requiring patients to be moved to a nearby outdoor parking garage — sometimes carried down flights of stairs to get there.
And to think, Touro was in better shape than any other hospital in the region.
Within days, the hospital was evacuated, and the health care system had purchased four homes so its employees — many of which had lost theirs — had a place to stay. Hirsch led a recovery effort at Touro that saw it reopen just 28 days after Katrina, the first hospital in the area to do so.
Hirsch not only stayed through the re-opening, but for much of the initial rebuild of the area. He was at Touro for three years before returning to New Jersey to lead Saint Clare’s Hospital in Denville.
On the 20th anniversary of the most destructive Hurricane in U.S. history, Hirsch recalled many of the moments — and how it helped him lead during Superstorm Sandy and the pandemic.
Here’s more of an hour-long conversation with BINJE.
BINJE: You’re a Jerseyan, someone who had risen in the ranks to become CEO at Cooper Health before leaving there to take a similar job at Exempla-Saint Joseph Hospital in Denver. You had just agreed to become the new CEO at Touro in 2005. Take us through that first week on the job?
Les Hirsch: I started on Monday, August 22. Within a few days on the job, our focus turned to Katrina. We knew it was coming but we didn’t know how big it was going to be. The storm first made landfall in Florida and moved across the state, and then it plopped in the Gulf as a Category One. But then it just exploded into a Category Five and took a big hook and turned North. By Thursday of that week, it was clear that the models were showing that it was coming toward the Gulf Coast and that it was targeting New Orleans.
BINJE: You were new to the area and to hurricanes. What was the view of the longtime employees there?
LH: Historically, what they did in New Orleans during a hurricane was just hunker down and ride it out. Then life gets back to normal pretty quickly. We were focused on Katrina on Thursday, but as it got closer, it was very clear to all employees it was going to be big. By Saturday and Sunday, we knew that we were in the crosshairs.
We started to feel the effects of the storm in the middle of the night. By 3:30 on Monday morning, we had lost power. Fortunately, at the very end, the storm veered a little bit to the east, so we were spared a little bit. And by 11 or 12 o’clock that morning, the sun came out. We thought we were in good shape. We figured we had dodged a bullet. Then the levees broke. That made it exponentially worse.
 BINJE: What did you do next?
BINJE: What did you do next?
LH: People told me we could have up to 10 feet of water, which was just unfathomable to me. That didn’t happen, though we did move our command center temporarily upstairs. But when the generators started to fail, right after we got a shipment of fuel, we couldn’t overcome that.
It was like being on a ship that was starting to go down. If you lose generator power, you literally have nothing. You have no HVAC. You have no power in critical care units. We had patients on ventilators that had to be manually bagged. Then we lost the water supply. We had no potable water or water pressure.
We had a high risk of loss of life so it was clear to me that we would have to evacuate the facility. But that brought a different challenge.
BINJE: How so?
LH: All of our communications were cut off. There was just no contact with the outside world. Cell phones weren’t working. Cable TV was down. I finally was able to make a phone call on the one phone that was working: A pay phone in the emergency department.
I called John Matessino, the president of the Louisiana Hospital Association, who I had met during my interview process at Turo. I learned the association had set up its own command center in Baton Rouge. John became our lifeline to the outside world. By Tuesday afternoon, he connected us to Acadian Ambulance Service, the largest private medical ambulance company in the country, one that had ambulances and helicopters. We were going to evacuate.
BINJE: Talk about that process?
LH: First, we had to get people out of the hospital. Without electricity, it became too hot. So, we moved them to a parking garage that was connected to the building. We literally had to carry some people down the stairs, but we had to get them out of there. It was still hot outside. Even at night, the heat index was in the 90s, but it was better than inside the hospital.
We were preparing to evacuate the neonatal intensive care unit that night, but we couldn’t get the helicopters because it was so dark. Remember, New Orleans was dark. All the lights were out. So, we had to put it off until Wednesday morning.
 It was a frenetic time. I can remember having names on a whiteboard. We were literally triaging the patients in the hospital in terms of setting priorities to evacuate people, by air and by land. We got the babies out first but that was complicated. In many cases, there were no parents. But we had to get them out. Some went to the northern part of the state, some of them went to Houston. And remember, we didn’t have electronic health records like we have today. So, we were packing up patients with charts. But once they left Touro, we had very little ability to know where they went.
It was a frenetic time. I can remember having names on a whiteboard. We were literally triaging the patients in the hospital in terms of setting priorities to evacuate people, by air and by land. We got the babies out first but that was complicated. In many cases, there were no parents. But we had to get them out. Some went to the northern part of the state, some of them went to Houston. And remember, we didn’t have electronic health records like we have today. So, we were packing up patients with charts. But once they left Touro, we had very little ability to know where they went.
We were moving rapidly. And then, at about 1 p.m., it all stopped.
BINJE: What happened?
LH: All air support was called to rescue people off their roofs. People were drowning in their attics. They had to help them. That was the situation we were living in. And it only got worse. If you remember, about 30,000 people had gone to the Superdome, and the situation there got bad quickly. People were fed up. The conditions were horrible. There were reports of all kinds of civil unrest.
BINJE: Talk about the civil unrest and how it impacted your situation?
LH: I don’t want to paint a picture that people are bad. The fact is, the government failed. Katrina tilted the pinball machine. This was something that happened that no one had ever expected, had ever experienced or had ever planned for. It caught the government at the city, state and federal level flat footed. People suffered great hardship. That influenced some of the behaviors that occurred there.
We started to hear all the stories. We were worried the civil unrest would come here. In fact, the fire commissioner, who was at Touro because his wife worked here, said, ‘We might have to leave some patients behind.’
I wasn’t going to do that.
I told him, ‘That’s not going to happen. We’re not going to leave here until we get every patient out.’ I said, ‘If you have that authority and you want to relieve me, then you can do that, but we will not leave here until we evacuate the entire facility.’
 We eventually got everyone out by Thursday morning, but by the time we left, we literally had an armed perimeter around the hospital.
We eventually got everyone out by Thursday morning, but by the time we left, we literally had an armed perimeter around the hospital.
BINJE: What were the next steps?
LH: Several of us on the leadership team went to Baton Rouge on Thursday afternoon, our chief of security lived there. Over the weekend, I went out and bought four homes on behalf of the hospital, sight unseen, because a real estate frenzy started to occur and we needed a place where we could house staff. We had about 30 people living in those homes.
And even before we evacuated, I was already in discussion for a temporary office location adjacent to the hospital association office in Baton Rouge. And I was working with a firm in New Jersey to build an emergency website.
We were moving from disaster to recovery. Incredibly, we were able to move back into the hospital 28 days later. We were the first hospital to reopen.
BINJE: During the recovery, you made a brief return to Colorado. Did you ever think about staying there?
LH: There was never any question in my mind that I was going back. But when I did come back to New Orleans, I remember our board chair, Steve Kupperman, kept thanking me for returning. I finally said, ‘Steve, did you really think I wasn’t coming back?’
He said, ‘Why should you? You don’t have a stake here.’
I didn’t see it that way.
I said, ‘I know you don’t know me that well yet, but we’re going to get to know each other a lot better.’
BINJE: There are so many executive lessons that can be learned from this. Give us a couple?
LH: As leaders, we have to deal with things that we’ve never dealt with before – whether it’s an incredible natural disaster or a pandemic. In those cases, I’ve found instincts are very important. When you’re under duress, you need to draw on your experience as a frame of reference.
And along with instincts comes courage, tenacity and the ability to have a mental toughness. You need to have the ability to think clearly and not get caught up in the emotion of the moment. If everybody else is freaking out, you cannot join them. You have to have the ability to take a step back emotionally and approach these things in a calm and measured way. Thank God, I have the ability to do that.
Now, I’m not saying that I never feel a rapid heartbeat, or I don’t have feelings, but as a leader, you cannot get caught up in the emotion of the moment.
BINJE: Of course, Katrina was like nothing any hospital had ever seen. Take us back to those days, try to describe the emotion of the moment?
LH: I remember the sense of fear. I remember all the hardship and the suffering that people on the staff went through. So many people had lost their homes or were worried they were going to lose their homes. Some lost even more.
I remember speaking with a housekeeper, just asking her how things were going. She told me how she had lost her husband, that he had drowned in the attic of their house. I’ll never forget that.
I’ll always remember the real human impact that occurred in this situation — and how it happened because of a complete failure of government. Hopefully, that will never happen again.
BINJE: Final question. Milestone moments impact people in different ways. How do you intend to mark the 20th anniversary of Katrina? What will that day be like for you?
LH: I’ll be thinking about the people there that mean so much to me. I can tell you that every year on that day there are a couple of people that I always speak to. Lately, I’ve found myself often looking at pictures from that time, remembering all that went on. I know that a chill will come over me.